If you’ve been dealing with chronic joint pain, you’ve probably heard the usual advice. Rest more. Take anti-inflammatory medications. Try physical therapy. Maybe get a cortisone injection that works for a few months, then the pain comes roaring back.
The cycle gets exhausting. You’re not looking for temporary relief anymore. You want your joints to actually heal.
Stem cell therapy represents a different approach. Instead of just masking pain, this regenerative medicine technique aims to support your body’s natural repair mechanisms at the source of the problem.
Let’s walk through what stem cell injections actually are, what the research suggests, and what you should know before considering this option for your chronic joint pain.
What Are Stem Cell Injections?
Stem cell injections deliver concentrated cells derived from your own bone marrow or fatty tissue directly into a damaged joint. These aren’t cells from another person or a lab-grown culture. They come from your body.
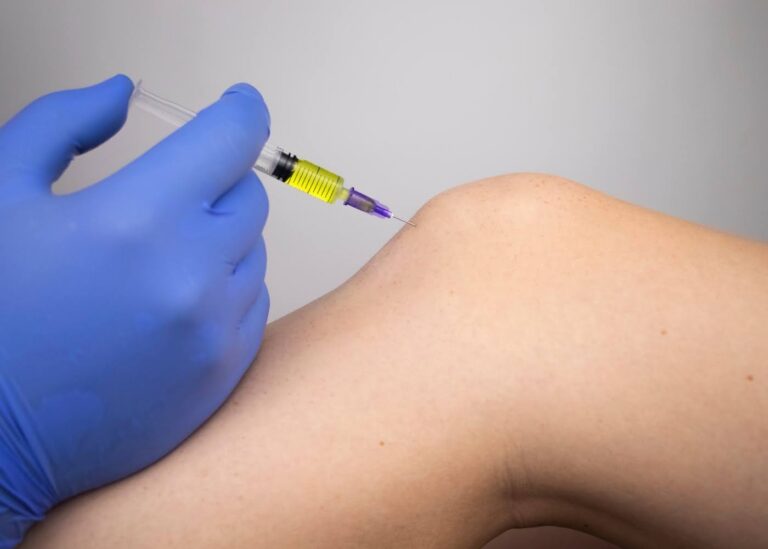
When doctors perform a stem cell injection, they typically extract a small sample of bone marrow or fat tissue, process it to concentrate the beneficial cells, and then inject that concentrate into the joint using ultrasound or X-ray guidance for precision.
The idea is straightforward: the injected cells may reduce inflammation, support tissue repair, and potentially slow further deterioration in the joint.
How Stem Cells May Work in Damaged Joints
Stem cells work through multiple mechanisms:
- They secrete substances that reduce inflammatory signaling
- They stimulate your body’s own repair processes
- They support new blood vessel growth to improve healing
Here’s what many clinics miss: stem cells work dramatically better in a healing-supportive internal environment. If your body is chronically inflamed, hormonally imbalanced, or nutritionally depleted, even high-quality stem cells struggle.
At Rocky Mountain Regenerative Medicine (RMRM) in Boulder, we optimize your internal biology before and after injection to maximize results. Think of it this way, you can plant the finest seeds, but if the soil is depleted, they won’t flourish.
What Does the Research Say?
Research on stem cell therapy for joint pain is encouraging. Stem cell injections for knee osteoarthritis show promising results for pain reduction and improved function, with outcomes varying based on cartilage severity, age, and injection technique. Studies on hips, shoulders, and elbows show preliminary evidence, and a growing body of literature suggests stem cells may slow osteoarthritis progression.
Success depends on careful patient selection, precise technique, and optimization of overall health. Clinics that assess and optimize systemic health factors (inflammation, hormones, nutrition, metabolism) report better outcomes than those performing injections in isolation.
Conditions That May Respond to Stem Cell Therapy
Stem cell injections have been explored for a range of joint and musculoskeletal problems:
- Osteoarthritis of the knee, hip, shoulder, or ankle
- Chronic tendon injuries, such as tennis elbow or rotator cuff tendinopathy
- Cartilage damage from prior injury
- Ligament injuries that haven’t fully healed with conservative care
- Joint pain related to degenerative disc disease in the spine
Learn more about stem cell therapy for degenerative disc disease if spinal pain is your concern.
The treatments are individualized. A clinician evaluates your specific joint, imaging, medical history, and goals before recommending stem cell therapy.
Interested in comprehensive care that supports long-term health? RMRM offers annual memberships that provide ongoing access to regenerative therapies and wellness optimization.
The Procedure: What to Expect
Before the Procedure
Rocky Mountain Regenerative Medicine begins with a thorough evaluation before the injection, the most critical phase for maximizing results.
Your assessment includes a detailed health history covering past injuries, medications, family history, and lifestyle factors like sleep, stress, diet, and exercise. We also carefully review your imaging (X-rays, ultrasound, or MRI) to assess your specific joint damage severity.
Laboratory testing is a critical component, assessing inflammatory markers like CRP and homocysteine that indicate chronic inflammation, hormone levels (thyroid, sex hormones, cortisol) that directly influence tissue repair, metabolic markers (glucose, insulin, lipids) revealing your cellular energy and resources, and nutrient status (vitamin D, B vitamins, magnesium, zinc) needed for tissue repair. We also assess oxidative stress markers to understand whether your antioxidant defenses are adequate.
Beyond the numbers, we perform a physical examination assessing interconnected systems, recognizing that joint pain often relates to systemic factors far beyond the injured joint itself.
Based on your assessment, you may receive recommendations for hormone optimization, anti-inflammatory nutrition, targeted supplementation, or sleep and stress management, all of which improve your stem cell response.
On the Day of the Procedure
You’ll arrive for intake, and the procedure typically takes 1-3 hours total. Tissue harvest takes 45-60 minutes, where adipose extraction (procedure used at RMRM) is performed via a liposuction procedure under local anesthesia.
Your sample is then either sent directly to the lab for processing or is processed in the clinic for same-day injection to concentrate stem cells and growth factors, which takes 1-2 hours. Finally, the injection phase takes 15-45 minutes, where, using ultrasound or fluoroscopic guidance, the concentrated product is injected into your damaged joint with local anesthesia. You remain awake throughout the entire procedure.
After the Procedure
Standard aftercare includes limited activity for 48 hours, avoiding strenuous exercise for 2-4 weeks, applying ice or heat as directed, and engaging in physical therapy or gentle movement to support healing.
RMRM provides ongoing support to optimize your healing environment throughout recovery, including continued anti-inflammatory nutrition guidance, monitoring of sleep, stress, and inflammation levels, follow-up labs to verify biomarkers support tissue regeneration, and regular check-ins to adjust protocols and monitor your progress. We also integrate complementary therapies like peptide therapy, hyperbaric oxygen, or shockwave when appropriate for your specific situation.
Some patients report improvement within weeks; others take 2-3 months, and a few see continued improvement over 6 months. Timeline varies based on damage severity, age, overall health, and compliance with aftercare. Ongoing systemic optimization during recovery significantly extends results.
Is Stem Cell Therapy Right for You?
Consider whether you’ve tried conservative options like physical therapy, medications, or cortisone injections without adequate improvement, and whether your joint damage is confirmed by imaging. Ask yourself if you’re committed to the recovery timeline and have realistic expectations—stem cells may slow progression and reduce pain, but severe osteoarthritis responds less predictably.
Additionally, consider whether you’re willing to address systemic health factors like inflammation, hormones, and nutrition that affect healing, can commit to lifestyle modifications including sleep, stress management, and diet, and are ready to partner actively in your care rather than passively receiving treatment.
A qualified regenerative medicine provider can help assess your candidacy. If you’re wondering whether to pursue regenerative therapy or surgery, explore stem cell therapy vs. knee replacement to understand your full range of options.
Other Regenerative Therapies Worth Considering
Stem cell therapy is one tool among several. You may also benefit from:
PRP (Platelet-Rich Plasma): Uses concentrated platelets from your own blood to deliver growth factors to injured tissue. Often less expensive than stem cell therapy and sometimes used in combination with it.
Exosome therapy: A newer approach using extracellular vesicles from stem cell cultures. Learn more about exosome therapy benefits.
Hyperbaric oxygen therapy: May support tissue healing by increasing oxygen availability to damaged areas. Read about hyperbaric oxygen therapy uses to understand how it complements other regenerative approaches.
Shockwave therapy: Uses acoustic waves to stimulate healing in chronic tendon injuries.
Many regenerative medicine clinics offer combinations of these approaches tailored to your specific condition and goals.
Take the Next Step
Chronic joint pain doesn’t have to be permanent. Stem cell injections represent one option for supporting your joints’ healing capacity.
At Rocky Mountain Regenerative Medicine, we assess not just your joint but your entire healing capacity, your inflammation levels, hormone balance, nutrition, metabolic health, sleep, and stress. The best outcomes come from optimizing your complete healing environment alongside the regenerative therapy itself. This integrated approach is what distinguishes clinics achieving good results from those achieving exceptional ones.
Ready to learn more? Contact us to discuss your joint pain and explore whether regenerative therapy might help.
Schedule a Consultation | Book an Appointment